There’s More Than One Type of Pain. Scientists Are Learning to Treat Each of Them
The first squeeze of my left thumb is mild, nearly reassuring. I fee it as out of 100 on the soreness scale.
But as a technician ramps up tension on the tailor made-made thumb-squeezing device, it becomes considerably less nice. I give ratings of two, 6 … then 36. A several squeezes afterwards, I’m at 79.
At eighty four, I’m glad the check is about as I set my tender thumb to my lips.
I have available myself up for a soreness research at the College of Michigan, in a lengthy, reduced-slung setting up northeast of the university’s key campus in Ann Arbor. As the working day wears on, I’ll undergo needle pokes, leg squeezes and an MRI scan — all portion of a grand bid to better comprehend the root bring about of an individual’s soreness, and stage to the most effective answers.
It’s an comprehension that’s sorely desired. Blessed for me, I’m just a manage in this experiment, and I can cry for mercy each time I want. That is not the case for the multitudes of people — 50 million in the US on your own — who have ongoing, chronic soreness, for whom the health-related pause buttons are significantly from enough.
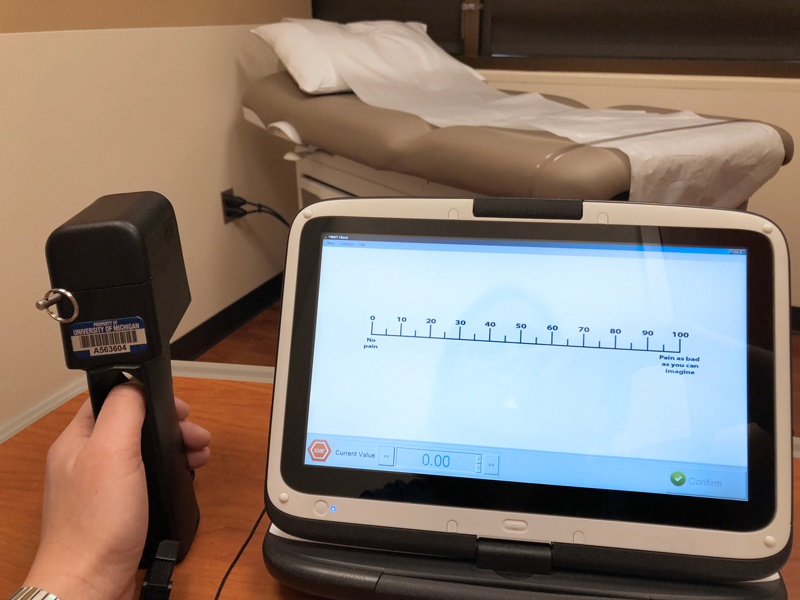
The thumb tension check, in which members fee their soreness amount on a scale from to 100 as their thumbs are subjected to raising tension, is just one of quite a few approaches that clinicians and researchers can examine a person’s soreness responses. Considering that people’s thresholds to soreness in exams like this change in accordance to soreness syndrome, this kind of exams can help with diagnosis. (Credit rating: Amber Dance)
“Our remedies for chronic soreness are quite poor,” claims Richard E. Harris, a neuroscientist at the College of Michigan’s Long-term Discomfort and Tiredness Exploration Middle and a co-researcher on the research, which ought to eventually help to strengthen diagnoses and therapies. These days, medical doctors typically define soreness by wherever it is: the abdomen, the lessen again, the joints. Then they offer up remedies, normally anti-inflammatories or opioids, that far too typically do nothing at all to the cells and molecules producing a particular person to harm. A the latest investigation in the Journal of the American Healthcare Affiliation found that opioids lowered soreness by an average of considerably less than just one stage on a ten-stage scale, across a selection of chronic problems.
As portion of the precision medicine movement and many thanks to contemporary brain-imaging engineering, scientists are setting up to puzzle out the distinct sorts of soreness: what leads to them, how to diagnose them and how to prescribe remedies to match. It’s an region that is significantly from settled. As lately as 2017, the Global Affiliation for the Research of Discomfort defined a new soreness variety, known as nociplastic. It’s characterized by the absence of any nerve or tissue hurt in the components that harm.
Dan Clauw, director of the Michigan soreness middle, is passionate about aiding people with this variety of lengthy-misunderstood soreness, which could underpin chronic problems, this kind of as fibromyalgia, that afflict thousands and thousands. His blue eyes flash guiding spectacles as he describes crisscrossing the world to teach other medical professionals about nociplastic soreness. He’s putting on a navy blazer and slacks when we fulfill for lunch in between my tests classes, since he’s just returned from offering a presentation about marijuana and soreness. He jokes that his colleagues will not recognize him out of his regular jeans.
Imaging the brain, together with undertaking prodding and poking exams of the variety I endured, is beginning to stage to signatures that demonstrate the challenge and counsel answers. Eventually, this expertise will help scientists to establish much more targeted therapies, so medical doctors can take care of clients superior.
Taxonomy of Discomfort
In wide strokes, soreness falls into 3 groups: nociceptive, neuropathic and nociplastic. (“Noci-” is from the Latin for “to do harm.”)
Nociceptive soreness outcomes from inflammation or direct hurt to tissues. When that torture device squeezes my thumb, for case in point, soreness-sensing nerves see the tension and spring into action. They transmit messages to my spinal wire, which sends them on to my brain, telling me “Ouch!”
This variety of distress is typically shorter-lived mine dissipates right after I have sucked on my thumb for a several moments. Nociceptive soreness can also be chronic, though — for case in point in osteoarthritis, wherever the cartilage in joints wears absent and leads to stretching of tendons and ligaments, or by the ongoing inflammation of rheumatoid arthritis.
Neuropathic soreness, in distinction, takes place when the soreness-sensing nerves them selves are destroyed or irritated, so that they mail inappropriate “Ow!” signals to the brain. It normally outcomes from some damage or disease, this kind of as diabetic issues or shingles. It can also occur when a nerve is pinched, as in the case of carpal tunnel syndrome, when a nerve in the wrist receives squeezed. It’s typically lengthy-long lasting, unless of course the hurt is fixed.
And nociplastic, the freshly named variety, outcomes from no apparent inflammation or damage. Fairly, it’s as if the quantity knob for soreness is turned up way far too higher, not at the soreness web-site alone but further more afield. Nociplastic soreness looks to come up in components of the central nervous process — the brain or spinal wire — that acquire, transmit or process those people “Ouch!” signals. These nerves misfire, developing a sensation of soreness even though nothing at all may be completely wrong. The locale of the challenge, the central nervous process, is why Clauw prefers to connect with it “central sensitization.” The basic case in point is fibromyalgia, which leads to soreness that looks to stem from muscle groups, tendons and joints, despite the real problem’s lying in the brain or spinal wire.

Scientists’ comprehension of soreness continues to evolve and so do the numerous phrases made use of to describe it. Ideally, definitions are standardized and mirror the biology underpinning the soreness, but the lack of easy exams for parsing sorts of soreness will make defining it a obstacle. Nociceptive soreness involves soreness-sensing nerves known as nociceptors, which also can be included in neuropathic soreness. A third soreness variety is considered to come up wholly in the central nervous process. But there can be overlap: Nociceptive and neuropathic soreness can, about time, lead to central nervous process-created soreness.
Complicating the picture, a particular person could possibly have much more than just one variety of soreness going on at the similar time. In 2012, the journal Discomfort published a case report of a particular person with burning, prickling soreness on both equally sides of the body. Procedure with pregabalin, an epilepsy medicine that can also address neuropathic soreness and central sensitization, relieved soreness on the appropriate aspect of the body, but not the left.
All this soreness classifying is much more than an educational workout: It ought to help guidebook how to take care of people. For case in point, take into consideration a individual with knee soreness. If the challenge is nociceptive, anti-inflammatories or knee operation ought to help. But if the challenge is central, those people remedies possibly will not make significantly big difference. A superior wager would be drugs that can immediately impact the misfiring central nervous process. Some antidepressants, for case in point, act on the brain’s chemical messengers — neurotransmitters — that are included in soreness, altering their signaling to quell the “Ouch” concept.
Non-drug remedies this kind of as acupuncture and cognitive behavioral therapy also may help since they impact how the brain perceives soreness. Acupuncture boosts availability of brain receptors that reply to the body’s all-natural painkillers. A the latest investigation in JAMA Internal Medicine of much more than 6,000 people taking opioids located that remedies this kind of as meditation, hypnosis and cognitive behavioral therapy reduced soreness and diminished the drug doses desired to manage it.
Grand Central Station
However the time period “nociplastic” is new, Clifford Woolf, a neurobiologist at Boston Children’s Healthcare facility and Harvard Healthcare School, first proposed the thought in 1983. But the idea has been sluggish to capture on. In the 1990s, when Clauw started studying fibromyalgia, it was a disease so obscure, so puzzling, that some medical professionals simply denied its existence.
These days, fibromyalgia is much more possible to be approved as a real situation. But numerous medical doctors however do not take pleasure in how centralized problems could possibly underlie soreness even when the symptoms appear nociceptive or neuropathic, Clauw claims. The distinctions in between soreness sorts are not clean up: If left untreated, nociceptive soreness may sensitize the nervous process, turning a momentary challenge into chronic, nociplastic soreness, for case in point. Clauw and his Michigan colleagues believe that central sensitization exhibits up in myriad problems, from irritable bowel syndrome to chronic pelvic soreness to dry eye disease. And in the research I have signed up for, they want to explain how typically this takes place and how medical doctors could possibly detect it in clients who present up begging for soreness aid.
To that conclusion, the crew has enrolled people with 3 distinct soreness diseases that feel, on the surface, to be nociceptive or neuropathic. The scientists will check their soreness right before and right after normal remedies. If the soreness is in truth central, the remedies shouldn’t operate — a disappointment for the members, but just one that could possibly sooner or later lead to superior comprehension and treatment for them and some others like them.
Two groups of subjects have what appears like nociceptive soreness: those people with osteoarthritis of the hip, who will acquire a hip substitution, and those people with inflammatory rheumatoid arthritis, who will be treated with contemporary drugs. A third team, people with carpal tunnel syndrome, depict neuropathic soreness and will get operation to acquire the tension on the nerve.
But if Clauw and his crew are appropriate, then some of these people will actually be suffering from central sensitization, rather of or in addition to the nociceptive or neuropathic challenge. Two manage teams will help tease that out: Persons with fibromyalgia will present the researchers what pure central sensitization appears like, and those people like me, with no chronic soreness, will depict the non-central state.

The main way that medical professionals measure soreness right now is to talk to a person how significantly they’re hurting. Identification of biomarkers from, for case in point, brain imaging or blood exams could present much more goal actions of soreness that would offer benefits in a selection of settings.
When all the knowledge are in, the researchers hope that soreness options shared by the people with fibromyalgia and the some others whose remedies do not operate will reveal a possible signature for central sensitization.
The obstacle is that there’s no simple blood check or X-ray that will distinguish just one variety of soreness from a further. “There’s no single measure that, by alone, will depict soreness,” claims Woolf, writer of a paper in the Once-a-year Review of Neuroscience about soreness prompted by problems in the sensory machinery. “We require a composite.”
Hurts So Excellent
To construct that composite, scientists need to resort to a selection of indirect actions, together with responses to the pokes and prods getting inflicted on me and other subjects.
This certain piece of the picture, known as quantitative sensory tests or QST, actions the threshold at which a particular person can sense a specified sensation — this kind of as tension, heat or cold — and when that sensation becomes painful. This can reveal how a person’s nervous process offers with soreness, and how that process could possibly be off-kilter. Unique flaws in nerves lead to precise adjustments in soreness responses, aiding scientists to distinguish just one soreness variety from a further.
It’s simple, but revealing. For case in point, in the case of the thumb-push check, a particular person with fibromyalgia would possibly start to sense soreness at all over 4 kilos of tension. Clauw, who has no chronic soreness of any stripe and is fairly soreness-insensitive, claims that he can handle up to about eighteen kilos of tension right before it becomes not comfortable. The average particular person would possibly start to sense bothered at all over 8 kilos.
Or just take a check wherever I’m poked in the forearm with a needle. The device retracts into the handle like a Hollywood unique-results knife, so it doesn’t pierce my pores and skin, but it doesn’t sense terrific — I fee it a seven out of 100. Then I get ten pokes in rapid succession. That hurts much more, at 32. This is a standard reaction, but if I experienced central sensitization, I would possible have located the ten-poke sequence significantly much more painful.
In addition to sorting out nociceptive or neuropathic from centralized soreness, QST also looks capable to reveal subtypes. In research published in 2017, 3 European consortia executed QST on 900 people with numerous soreness problems, all regarded to be neuropathic. The testing separated the subjects into 3 clusters, and the research authors predicted that just about every would be suited to distinct remedies.

Improved-outlined markers for distinct sorts of soreness could radically strengthen soreness administration. As revealed, it would allow for clients to be sorted into scientific trials that would reveal the most effective remedies for just about every soreness subtype. Final results of those people trials would help medical professionals take care of unique clients much more proficiently.
The first cluster was characterized by deficits in sensation to contact, heat or pokes that would typically be painful. This implies that central sensitization could possibly be guiding the soreness in some of these people, claims research coauthor Nadine Attal, a soreness expert at the Aid Publique-Hôpitaux de Paris. Opioids, antiepileptics or antidepressants (made use of for their results on soreness nerves, not temper) could possibly help, since they act in the brain.
The 2nd team was outlined by extraordinary sensitivity to sizzling and cold — like pores and skin when it’s sunburned, which places soreness-sensing nerves on higher alert. For this variety of neuropathic soreness, nearby, numbing drugs this kind of as lidocaine, Botox or capsaicin (a therapeutic substance from sizzling peppers) could possibly be the appropriate option.
Persons in the third team had been significantly sensitive to tension and pinpricks, and its users typically claimed soreness akin to burning or electrical shock. This was a much more advanced team, Attal claims she thinks topical drugs or antiepileptics could possibly help. But now that researchers have the groups superior outlined, they can immediately check drugs to come across what definitely will work most effective for just about every.
Photographs of Discomfort
Searching at the brain in soreness also can help scientists distinguish soreness sorts, even though the responses are not crystal clear-cut. There’s no just one, lone spot wherever soreness lights up the brain, claims Sean Mackey, chief of the division of soreness medicine at Stanford College in California. Fairly, the soreness reaction is dispersed across a circuit that encompasses quite a few brain areas.
In the afternoon of my working day as a soreness-research subject matter, I’m led to the university’s North Campus for an MRI. The technician slides me into a grey, Standard Electric-branded, upright donut about the dimension of a golfing cart. The outside is festooned with frolicsome animal stickers (numerous subjects from other research are kids), but these do nothing at all to allay the distress of lying completely however with my head in a vise for an hour and a half.
As I lie there, listening to the scanner’s inharmonious beeps, rumbles and alien-laser-gun sounds, I’m not thinking of something in certain. Nevertheless, particular components of my brain are inclined to draw blood at the similar time, suggesting that they’re performing in sync. These are known as networks.

Around half of people with rheumatoid arthritis practical experience soreness even when applying drugs that manage the inflammation. MRI scans of some of these clients reveal amped up connectivity in between two brain regions, the default manner network and insula. This brain connectivity also has been located in people with fibromyalgia, a chronic soreness situation with roots in the central nervous process. The discovery implies that fairly than inflammation on your own, a dysfunctional central nervous process can also engage in a purpose in the soreness of rheumatoid arthritis. (Credit rating: Graphic obtained and created from the Long-term Discomfort and Tiredness Middle with guidance from the FMRI laboratory at the College of Michigan)
One particular that Harris and colleagues are significantly interested in is known as the default manner network. It turns on when I’m at relaxation and my brain wanders to subjects involving myself: what I experienced for breakfast, most likely, or what I’m arranging for tonight as soon as my working day of soreness is about.
One more network they’re observing is the salience network, which lights up when a particular person notices a new sensation — say, the squeezing of their thumb — to decide which sensations are value responding to. It incorporates the insula, a pyramid-formed bit of brain that Mackey and some others have joined to soreness.
Ordinarily, the insula and the default manner network are not likely to act at the similar time. But Harris and colleagues learned that in people with fibromyalgia, they had been significantly much more possible to flash in synchrony.
That will make perception, claims Rob Edwards, a soreness psychologist at Harvard Healthcare School and Brigham and Women’s Healthcare facility in Boston. For a person dwelling with chronic soreness, the soreness can turn out to be a core portion of their identification. “The salience-associated risk intrudes on, and even usually takes about, the way that you feel about yourself,” he claims.
Painkillers, Personalised
It may be possible to undo that intrusion, though. Edwards is at the moment tests cognitive behavioral therapy, or CBT, in people with fibromyalgia. In no way is he suggesting that their soreness, or any soreness, is imaginary, but therapy can help people deal with soreness superior and even lessen it. “It’s all about imposing a perception of manage and mastery,” claims Bob Kerns, a soreness psychologist at Yale College in New Haven, Connecticut, who coauthored a paper in the Once-a-year Review of Scientific Psychology on psychological treatment for chronic soreness.
In the research so significantly, CBT looks to be disentangling the salience and default manner networks in some people with fibromyalgia. Edwards predicts those people people will also practical experience soreness aid.
Remaining capable to forecast who will profit from a specified treatment could make a substantial big difference not just for unique clients, but also in scientific trials for new soreness-aid medicine. If scientists check a soreness drug on 100 people, but only a fraction of those people subjects in fact have the soreness system the drug can take care of, the medicine will appear like a flop — even if it’s a celebrity for a certain subset of clients. This has “almost certainly” occurred in previous trials, Woolf claims.
Mackey envisions a foreseeable future in which soreness clients can be tested for the underlying challenge, most likely with the similar varieties of exams I underwent at the College of Michigan, plus numerous much more assessments. For case in point, scientists are analyzing nerve endings in compact pores and skin samples from soreness clients, and some others purpose to tease out the purpose of genetics in chronic soreness. Easy questionnaires can also help to recognize soreness sorts, all with this purpose of prescribing drugs tailor-made for a person’s precise taste of misery.
Drugs is not quite there but — in truth, only ten yrs back Mackey would have known as that situation science fiction. “Stay tuned,” he claims, “because it’s no longer science fiction. . . . We’re going to get there.”
As necessary by the College of Michigan Institutional Review Board, Amber Dance was compensated $275 for her participation in the research at the Long-term Discomfort and Tiredness Exploration Middle. She donated that amount to the American Long-term Discomfort Affiliation.
This report at first appeared in Knowable Journal, an unbiased journalistic endeavor from Once-a-year Assessments.
